Here's the short answer: a torn muscle can absolutely heal and return to full strength, and with the right rehab and training it can even become stronger than it was before the injury. But it doesn't happen automatically, and the word 'stronger' needs some unpacking. The muscle doesn't come back tougher just because it got damaged. What actually happens is a repair process, not a regeneration one, and whether you end up stronger, weaker, or somewhere in between depends almost entirely on what you do during recovery.
If You Tear a Muscle Does It Grow Back Stronger?
What a muscle tear actually is (and why the type matters)

The term 'muscle tear' covers a pretty wide range of injuries, from microscopic fiber damage all the way to a complete rupture, and lumping them together is where most people go wrong. Clinicians use a three-grade system to sort them out, and knowing which category you're dealing with changes everything about how you should respond.
| Grade | What's happening | Typical symptoms | General healing window |
|---|---|---|---|
| Grade I (mild) | Small, localized fiber tears; most tissue intact | Mild local pain, full or near-full range of motion, little to no swelling | A few weeks |
| Grade II (moderate) | Moderate tear; partial but significant fiber disruption | Noticeable pain, some strength loss, visible bruising, limited ROM | 2–3 months or longer |
| Grade III (severe) | Complete or near-complete rupture of the muscle | Severe pain, rapid loss of contour, major strength deficit, >50% ROM loss | Several months; sometimes surgery required |
There's also an important distinction between a true muscle strain or tear (caused by shearing forces, like a hamstring pop during a sprint) and the micro-damage that comes from hard training. Delayed onset muscle soreness, or DOMS, is technically muscle fiber disruption too, but it's a completely different animal. DOMS has no long-term consequences and is part of the normal adaptation cycle. A real muscle tear, especially Grade II or III, triggers a repair process that involves scar tissue formation, which is not the same as the clean adaptation you get from a tough workout.
Do torn muscles grow back stronger? The honest answer
Yes, but with a big asterisk. When a muscle tears, the body goes through three overlapping phases: inflammation (the first few days), proliferation where satellite cells and connective tissue fill the gap, and remodeling where the new tissue matures and reorganizes. The catch is that this repair process doesn't produce a perfect copy of the original muscle. The healed area contains a small amount of scar tissue, and scar maturation completes in roughly 10 days. But returning to pre-injury strength takes weeks to months even after the scar is structurally stable, because the new tissue needs mechanical loading to remodel and strengthen.
This is where the nuance lives. Studies using MRI and histology show that by around 4 weeks after a severe muscle injury, there's measurable interstitial fibrosis, meaning connective tissue has replaced what were muscle fibers. That tissue can adapt, but it's not the same as pristine muscle. So the mechanism for 'growing back stronger' isn't the tear itself, it's the deliberate progressive loading you apply during and after rehab. The injury doesn't make you stronger. Your response to the injury is what determines strength outcomes.
That said, plenty of people do come back from muscle tears at equal or greater strength than before, particularly after Grade I and moderate Grade II injuries. The reason is usually simple: the injury forces them to address weak links, do proper rehab, and load the muscle in a more structured way than they did before. The tear itself didn't cause the strength gain. The disciplined, progressive rehab did. A complete Grade III rupture is a different story, and realistic expectations matter there.
Signs of severity: when to rest and when to get checked out
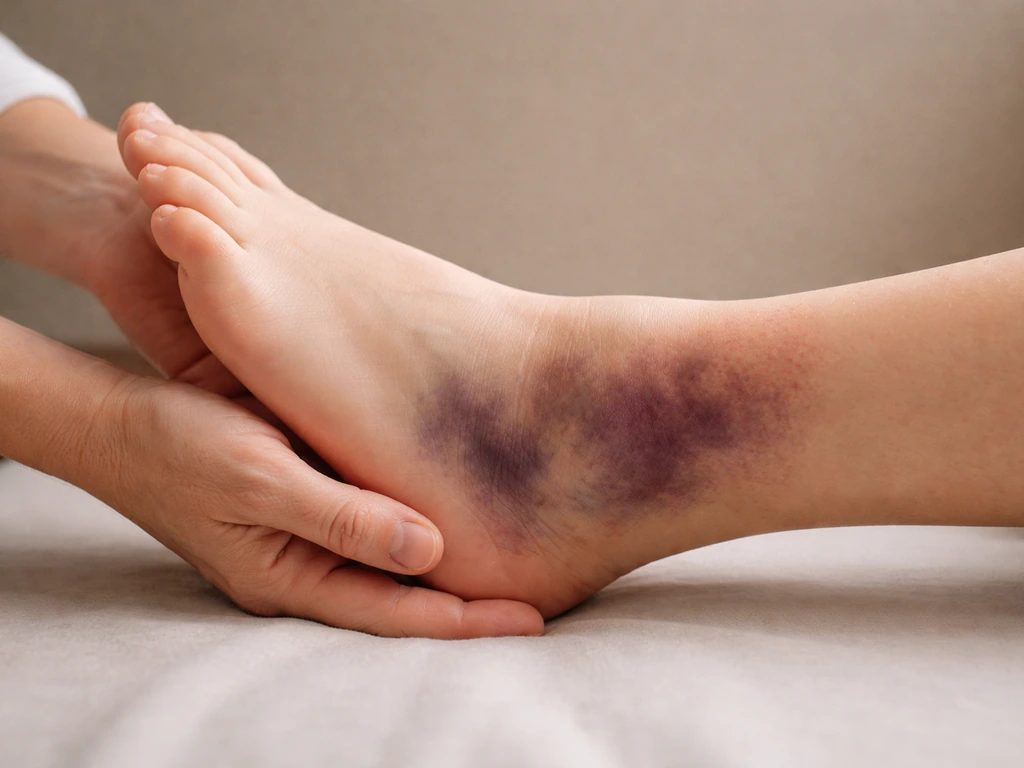
Most mild strains don't need a doctor visit, but there are clear signals that tell you to stop guessing and go get evaluated. Knowing the difference early saves you weeks of rehab time.
Rest and monitor at home if you have mild, localized soreness after a specific movement, can still move the joint through most of its range (even if it's a bit sore), have no significant swelling or bruising within the first hour, and can bear weight or use the limb with some discomfort but no sharp pain.
Get medical evaluation if you notice any of the following:
- A sudden 'pop' or snap felt or heard at the moment of injury
- Immediate significant weakness or inability to use the limb or bear weight
- Visible deformity, muscle bunching, or a sudden change in the muscle's contour
- Rapid, large-area bruising appearing within minutes
- Loss of more than half your normal range of motion
- Numbness or tingling in the area or down the limb
- Pain that is severe and not improving at all within 24–48 hours
A doctor can clinically assess your injury and, if needed, order imaging. High-resolution ultrasound is actually quite sensitive for muscle injuries, comparable to MRI at the 2–48 hour window after injury, and it's faster and cheaper. For suspected Grade III injuries or anything near a tendon attachment, imaging matters because the treatment path changes significantly.
What to do today: early recovery that doesn't backfire
The first 48–72 hours after a muscle tear are about protecting the injury, reducing unnecessary inflammation, and not making things worse. This isn't the time to push through or test your limits.
The basics in the first 48 hours
- Relative rest: stop the activity that caused the injury and avoid movements that reproduce the pain. You don't need to be completely immobile, but you do need to protect the area.
- Ice: apply a cold pack for 15–20 minutes at a time, up to 2–3 times per day in the early hours (some guidance suggests up to once per hour in the first day if tolerated). Keep a cloth between the ice and skin.
- Compression: a firm (not tight) wrap around the injured area helps limit swelling.
- Elevation: if it's a limb, get it above heart level when you're resting.
- Avoid NSAIDs in the first 48 hours if you can: some doctors advise against aspirin and ibuprofen in the initial window due to bleeding risk at the injury site. Acetaminophen for pain is a safer early choice if you need it.
After 48–72 hours, if swelling has decreased, gentle heat before light movement or stretching can help loosen stiff tissue. That said, you don't need to alternate ice and heat compulsively. Ice is most useful in the acute inflammatory window; heat is mainly helpful later for warming scarred or stiff soft tissue before movement.
Pain-guided movement: the principle you need to follow
Once the acute phase settles, the goal shifts from protection to active recovery. 'Pain-guided movement' means you move the injured area gently and only within a pain-free or nearly pain-free range. You're not pushing through sharp pain. You're using your body's feedback as the throttle. Gentle range-of-motion work in the first few days prevents excessive stiffness, maintains blood flow, and gives the healing tissue the low-level mechanical signals it needs to organize correctly. Total immobilization is not your friend beyond the first day or two.
How to actually rehab back to lifting: the phased approach
Rushing back to training is the single most common reason people end up with a nagging injury that lingers for months. Here's how to phase your return in a way that gives the tissue the stimulus it needs without overloading a repair zone that isn't ready.
Phase 1: Protection and pain-free ROM (days 1–14 for mild injuries)
Focus on restoring full range of motion without pain before you add any meaningful load. Gentle stretching, pain-free isometric holds (contracting the muscle without movement), and light bodyweight movements are your tools here. You are not training. You are signaling the tissue to heal in an organized way. For Grade II injuries, this phase will last longer, and for Grade III you'll likely be working with a physio from the start.
Phase 2: Progressive loading (weeks 2–8, grade-dependent)
Once you've got full or near-full pain-free ROM, you can start adding load. Begin with light resistance through a full range of motion, prioritizing eccentric control (the lowering phase of a movement) because eccentric loading is particularly effective at stimulating scar tissue remodeling. Increase load gradually based on your pain response, not on a fixed weekly schedule. If a load causes more than mild discomfort, it's too heavy right now.
Phase 3: Return to training (weeks 6–12+, grade-dependent)
Return to your normal training program only when you meet objective criteria, not just when you feel 'mostly okay.' Research on hamstring injuries (one of the most studied muscle tears in sport) lists these benchmarks: pain-free and symmetrical range of motion on both sides, no pain during maximal-effort isometric contractions, and limb symmetry in strength of at least 90–100% compared to the uninjured side. These aren't arbitrary numbers. They reflect tissue readiness. Clearing yourself early because the pain has faded is how re-injuries happen.
It's also worth noting that MRI or ultrasound can still show residual edema or signal changes even after you feel pain-free, which is one reason early return decisions based purely on symptoms can be misleading for more serious tears.
What you eat during recovery matters more than most people think
Muscle repair is an active biological process, and it runs on the same raw materials as muscle building. Nutrition and sleep are key factors in whether your muscles grow during recovery. If you under-eat or under-recover during the healing window, you are directly limiting the quality of the repair. Here's what the evidence actually supports.
Protein: the non-negotiable
Adequate protein intake directly increases muscle protein synthesis during recovery. Research on protein supplementation combined with rehab after acute muscle strain injuries shows it can support muscle volume recovery during the healing process. A general target of 1.6–2.2 grams of protein per kilogram of bodyweight per day is a solid framework during injury recovery, similar to what you'd aim for during active muscle-building phases. Whey protein is well-studied here: a randomized trial found that high whey intake after intensive eccentric exercise (a controlled version of the same kind of damage a tear creates) measurably reduced muscle damage markers compared to controls. Pea protein showed intermediate effects in the same study. Spread your intake across 3–4 meals rather than concentrating it in one sitting.
Total calories: don't cut while you're healing
This is not the time to run a calorie deficit. Tissue repair is energetically expensive. Your body needs adequate calories to fuel the inflammatory and rebuilding process, and cutting calories slows healing. If you're less active because of the injury, your needs are somewhat lower than normal, but you still want to be at maintenance or slightly above it, not in a deficit. Prioritize whole foods, micronutrient density (especially zinc, vitamin C, and magnesium which support connective tissue repair), and consistent hydration.
Sleep: probably your most powerful recovery tool
This one is underrated. A study in physically active soldiers found that those sleeping 4 hours or less had about 2.35 times higher likelihood of musculoskeletal injury compared to those getting 8 or more hours. Sleep deprivation also directly impairs acute skeletal muscle recovery after exercise. During an active injury, aim for 8–9 hours if you can get it. Growth hormone, which peaks during deep sleep, is one of the key drivers of tissue repair. Cutting sleep to get more workouts in while injured is a terrible trade.
Realistic timelines: what 'stronger' actually looks like
Let's be direct about timelines, because optimism about recovery speed is one of the main causes of re-injury.
| Injury Grade | Return to pain-free daily activity | Return to full training | Realistic strength outcome |
|---|---|---|---|
| Grade I | Days to 1–2 weeks | 2–6 weeks with proper loading | Full recovery common; can exceed pre-injury strength with structured rehab |
| Grade II | 3–6 weeks | 2–3 months or longer | Full recovery possible; requires disciplined phased rehab and nutrition |
| Grade III | Variable; often 6–12+ weeks | Several months; sometimes post-surgical | Highly variable; some recover fully, others have residual deficits; medical guidance essential |
The word 'stronger' after a tear is really shorthand for three separate things coming back together: range of motion, load-bearing capacity, and actual force output. These don't all return at the same rate. Range of motion typically comes back first, followed by capacity to handle load, and maximal strength last. Scar tissue, while structurally stable by around 10 days, continues to remodel and adapt for weeks and months. That remodeling is responsive to mechanical loading, which is exactly why progressive rehab isn't optional, it's the mechanism.
One thing worth being honest about: a complete rupture or a poorly managed Grade II tear that develops significant scar tissue may never return the muscle to exactly the same state it was in before. That doesn't mean you can't be strong, functional, and pain-free. It means that for severe injuries, 'stronger' may mean better overall function and greater surrounding muscle development rather than the exact fiber composition returning to baseline. That's a realistic but still genuinely good outcome.
There's a related question worth addressing here: strained muscles (a category that overlaps with Grade I and lower Grade II tears) follow a similar but somewhat more favorable repair trajectory, and the principles are the same. By following the same rehab principles, you can improve the odds that strained muscles recover in a way that supports strength gains. The core variables that determine the outcome, load timing, nutrition, sleep, and progressively rebuilding strength, apply across the spectrum of muscle injury severity.
Your actual next steps
If you're dealing with a muscle tear right now, here's what to do in order. Assess severity using the red flags listed above. If any of them apply, see a doctor before doing anything else. If it looks like a mild to moderate strain, start relative rest and ice today, keep the area moving gently within a pain-free range, and get your protein intake up to at least 1.6 grams per kilogram of bodyweight. Sleep as much as you can manage. Once acute pain settles (usually within a few days for mild strains), start light pain-free movement and work progressively toward loaded exercises over the following weeks. Don't return to full training until you have symmetrical range of motion and near-equal strength on both sides. That's the protocol that actually gets you back stronger. If you are wondering, do tattoos grow with muscle, the change in size or appearance usually comes down to how your skin and the tattoo stretch as your body changes. Tendons do not grow like muscles, but they can adapt with progressive loading during rehab do tendons grow like muscles. Do veins grow with muscles? In most cases, what changes is blood flow and vessel function with training, not that new veins permanently sprout in proportion to muscle size.
FAQ
How long does it usually take to feel like the muscle is “back to normal” after a tear?
Most people regain useful range of motion within weeks, but true strength often lags behind. A common pattern is ROM first, then load tolerance, then maximal force last. Even when tissue looks stable on the inside early on, the remodeled repair can keep changing for weeks to months, so feeling better does not always mean you are fully ready for heavier training.
If a tear is healed, why does it still feel weak when I go heavy?
Because “healed” tissue can be mechanically stable yet not fully capable of producing peak force. Scar-containing regions and altered tissue architecture often require time under progressive eccentric and loaded work to restore force output. Also, your nervous system and the surrounding muscles may not be retrained yet, so strength feels different even when pain is low.
Should I completely avoid training the injured muscle until I’m pain-free?
Not usually. The goal early on is to move within a pain-free or nearly pain-free range, using gentle, controlled motion to prevent stiffness and provide low-level mechanical signals. What you avoid is sharp pain, repeated testing, and heavy loading too early. If pain is rising day to day, that is a sign you progressed too fast.
What makes a “good rehab” different from just resting until it feels better?
Rehab is structured loading over time, not passive waiting. If you rest without rebuilding range and then gradually reintroducing resistance, the repair zone can remodel less effectively and you may end up with lingering weakness or stiffness. A good plan also uses objective readiness checks (like symmetrical ROM and tolerated isometrics), not just symptom relief.
Can I use stretching right away after a tear?
Early stretching can be helpful only if it stays gentle and pain does not spike. Aggressive stretching early can irritate healing tissue, especially for higher-grade injuries. As a rule, use pain-guided range-of-motion first, then progress to longer, slightly deeper stretching once swelling has calmed and you have near-full comfortable ROM.
Why do re-injuries happen even when the original pain is gone?
Symptoms can settle before tissue capacity fully returns. MRI or ultrasound findings like residual edema or connective tissue changes can persist even after you feel fine, and strength benchmarks may still be below readiness. Rushing return, especially into sprinting, heavy eccentrics, or long-duration load, is a frequent cause.
What are the most useful “objective” return-to-training tests I can do at home?
You can start with simple checks such as near-symmetrical ROM compared to the other side, pain-free or minimal pain during maximal effort isometric holds, and limb strength that is close to symmetrical. If you cannot perform controlled isometrics without pain, or ROM is still clearly limited, it is usually too early for heavy load or speed work.
Does protein intake affect muscle repair only, or also soreness and recovery?
Adequate protein mainly supports muscle protein synthesis and the rebuilding phase, which can indirectly improve recovery quality. It will not instantly erase pain, and it does not replace progressive rehab. The practical detail is spreading protein across 3 to 4 meals and aiming for a higher daily total during the injury window.
Is it okay to take painkillers to help me train through a tear?
Painkillers can mask signals, which may lead you to load too aggressively. Even if you feel okay, you can still exceed the tissue’s capacity during repair. If you consider medication, it is best discussed with a clinician who can balance pain control with safe progression and rule out higher-grade injury.
If I tear a muscle near a tendon, does recovery follow the same rules?
Tendon-adjacent injuries often change the timeline and the rehab approach. The attachment site is more sensitive to overload, and imaging is more important if a rupture at or near the tendon is suspected. In those cases, you may need a slower progression into stretching and heavy eccentric training to protect the insertion.
Does scar tissue mean I will never get stronger than before?
Not necessarily. Scar tissue can still remodel and handle increasing load, but it may not replicate the original tissue perfectly, so the exact “same muscle” outcome is not guaranteed. Many people do regain equal or greater function, and strength gains are typically driven by how well you restore ROM and progressively load during remodeling rather than by the initial injury itself.




